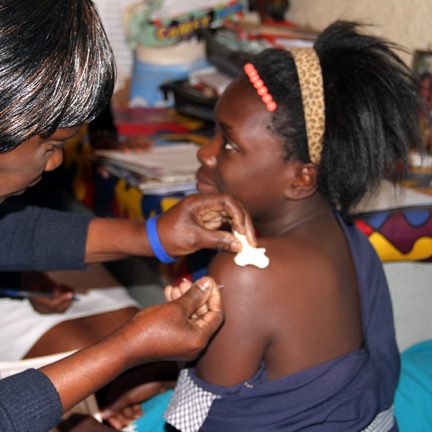
Rwanda's national HPV launch (2011)
April 2011What Happened
Rwanda became the first African country—and the first low-income country anywhere—to introduce HPV vaccination at population scale, after President Paul Kagame's government negotiated direct access to Merck's Gardasil. In its first round, 93,888 sixth-grade girls received the vaccine, reaching 95% coverage.
Outcome
Rwanda demonstrated that high HPV coverage was achievable in a low-income setting, contradicting the assumption that the vaccine was only viable for wealthy countries.
Subsequent surveillance showed HPV-16/18 infection rates in vaccinated cohorts falling sharply, providing the first hard evidence that the vaccine works at population scale in sub-Saharan Africa and giving every later rollout a working template.
Why It's Relevant Today
Burundi's launch follows the operational model Rwanda established 15 years earlier: school-based delivery anchored to a specific girls' age group, with community outreach for those outside school. Rwanda showed it could be done; Burundi is one more country choosing to do it.